Lupus and Antiphospholipid Syndrome
A lupus diagnosis can be confusing and scary enough, let alone being diagnosed with antiphospholipid syndrome as well. Learn about this condition that affects up to 50% of individuals with SLE.
.
- Introduction
- Signs and Symptoms of Antiphospholipid Syndrome
- Antiphospholipid Syndrome Causes
- Antibody Profile of Antiphospholipid Syndrome
- Diagnosing and Treating Antiphospolipid Syndrome
- Complications of Antiphospholipid Syndrome
- Managing Antiphospholipid Syndrome
- In Conclusion
Introduction
Antiphospholipid syndrome (APS) – also known as Hughes syndrome, lupus anticoagulant and phospholipid antibody syndrome – is an autoimmune disorder that is characterized by excessive clotting of blood in the arteries and veins. Normally, blood clotting happens naturally as the body’s response to cuts, scrapes and small breaks in blood vessels. In APS, however, a tendency for excessive clotting can constrict or even block blood flow and end up damaging internal organs. This can be a difficult condition to identify, as many individuals will not show signs of APS until they develop corresponding health problems at the organ level and blood tests confirm the presence of specific autoantibodies.
What does “antiphospholipid” mean, and how does APS relate to lupus? The term “antiphospholipid” refers to the target of the autoantibodies that are mistakenly produced by the body. Phospholipids are a special kind of molecule (part fatty acid and part phosphate group) that make up cell membranes in the body. It is the layer of phospholipid molecules that both hold cells together as well as support all the proteins that identify each cell and allow them to function. When the immune system produces antibodies that attack these very important molecules, they are called antiphospholipid (aPL) antibodies. The phospholipids and associated proteins in the blood (such as one called β2-glycoprotein-I) also attract these antibodies, and this begins the thickening and clotting of blood in normally healthy vessels. As with lupus, it is the body’s own immune system that causes the damage.
There are two types of APS:
- Primary APS: The individual has no known autoimmune disease present, other than APS. This type accounts for more than 50% of all cases.
- Secondary APS: The individual has already been diagnosed with systemic lupus erythematosus (SLE) or another underlying immune disorder. More women than men have this type of APS which matches the statistics for SLE and other overlapping connective tissue diseases.
Having a better, general understanding about what APS is and how to manage it may help take some of the fear and ambiguity out of the condition itself, especially when already trying to cope with lupus.

Signs and Symptoms of Antiphospholipid Syndrome
If an individual has lupus, they may want to speak with their practitioner preemptively to see if they are at risk for developing APS and if they should get tested for the presence of the antibodies. Conversely, if an individual has been recently diagnosed with APS, they may want to get tested to see if they have any other autoimmune disorders as well.
The signs and symptoms of APS include:
- Signs of deep vein thrombosis: Pain, tenderness, redness, or swelling in your leg or arm. This is the most frequently reported sign of APS.
- Signs of a stroke: Numbness, weakness, or paralysis of your face, arm, or leg, impaired vision, or sudden and severe headache, or difficulty with speaking or understanding speech.
- Signs of a pulmonary embolism (when one or more arteries in your lungs become blocked): Pain or shortness of breath, chest pains that worsen with deep breathing, cough that may produce bloody or blood streaked sputum.
- Unexplained bleeding: Any unexplained bleeding from the nose or gums, unusually heavy menstrual cycle, black or bright red stool, vomiting that looks like coffee grounds or is bright red. If you are pregnant and experience spotting or bleeding, this may be a sign of a miscarriage or other pregnancy complications.
These conditions require immediate medical attention. Individuals should reach out to a healthcare practitioner as soon as possible.
Antiphospholipid Syndrome Causes
Like most autoimmune diseases, the definitive cause of antiphospholipid syndrome remains unknown. What is known is that the body is encouraged to produce antibodies that target the proteins that bind to the phospholipids.
Factors that may be associated with developing APS include:
- Infections: Infections like HIV, syphilis, Hepatitis C, Lyme disease do have a higher incidence of having antiphospholipid antibodies.
- Medications: The antibiotic amoxicillin, hydralazine taken for high blood pressure, quinidine which is taken for regulation of heart rhythm and the anti-seizure medication phenytoin may lead to a higher risk for the development of antiphospholipid antibodies.
- Genetics or Heredity: Research indicates that relatives of those with antiphospholipid syndrome have an increased likelihood of having the antibodies themselves, even though the disorder is not considered to be hereditary.
- The presence of other autoimmune diseases: Individuals with other autoimmune diseases such as lupus may be at greater risk for developing APS.
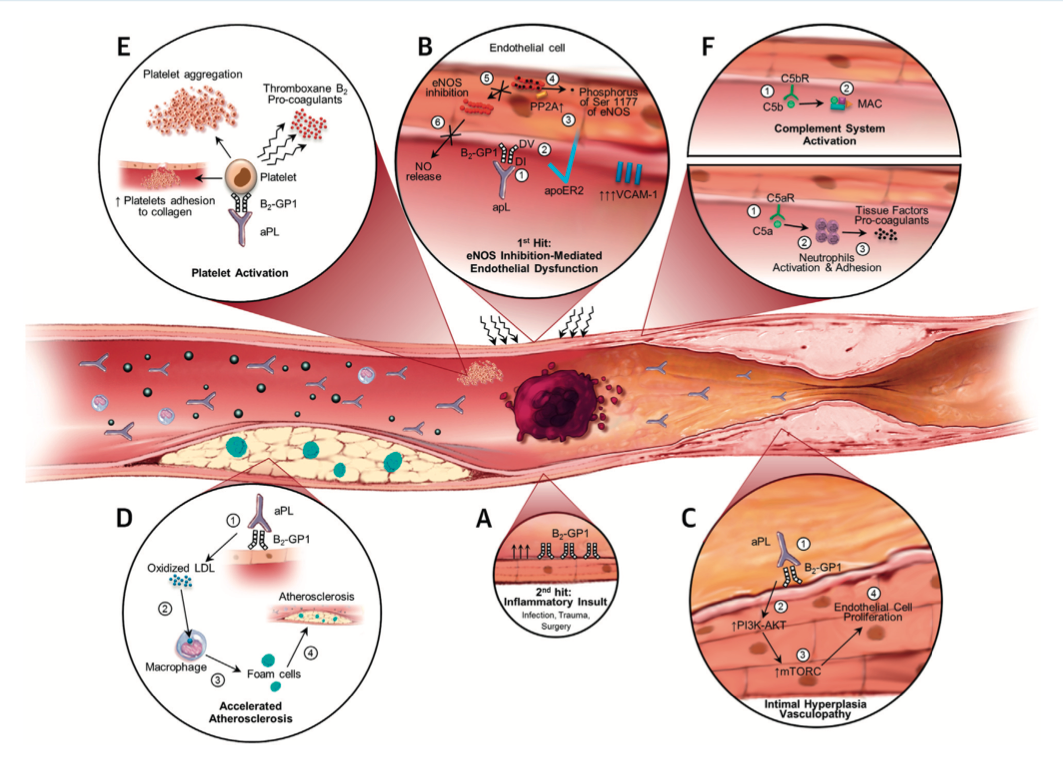
Antibody Profile of Antiphospholipid Syndrome
The antibody profile when APS is present includes:
- lupus anticoagulant (LA);
- anti-beta 2 glycoprotein a (anti-ß2 GP1);
- anti-prothrombin;
- immunoglobin G (IgG); and
- anticardiolipin antibody (aCL) including immunoglobin M (IgM) anticardiolipin antibody.
An aCL test used to test for syphilis can read as a “false positive” syphilis test for someone with pre-existing autoimmune disease who is being tested for APS. In these circumstances, aCL can indicate the presence of APS with other autoimmune diseases such as lupus. Because an aCL test is not so specific, it should be given at the same time as testing for anti-ß2 GP1 and LA in order to more definitively determine APS.
Diagnosing and Treating Antiphospholipid Syndrome
Most likely, a professional specializing in vascular disease, obstetrics or hematology will diagnose and treat APS along with a team of healthcare practitioners who will work to manage an individual’s lupus symptoms and other conditions.
Diagnosing APS
In 1998, researchers developed classification criteria for APS that was revised in 2006. The criteria includes:
- the presence of a lupus anticoagulant (LA), and/or
- medium to high titers of IgG or IgM; and/or
- a high titer of anti-ß2 GP1.
A blood test called a partial thromboplastin time (aPTT) test that looks for LA, aCL and anti-ß2 GP1 antibodies. This test measures how long it takes clotting to occur in a test tube of plasma. A prolonged PPT test means that there is a deficiency of clotting factors due to the presence of the antibodies for APS.
A diagnosis will be confirmed after the antibodies appear in blood at least twice consecutively in tests that are taken at least 12 weeks apart.
Treating APS
The treatment plan will be specific to the individual and their current health status with regards to the APS symptoms that they are experiencing. Ideally, any treatment regimen will be directed towards thinning (anticoagulating) the blood to prevent clotting.
If an individual is asymptomatic and has not experienced any complications as a result of APS, they may not be prescribed any medications and instead monitored regularly for changes over time. If an individual is asymptomatic, but has a high risk of cardiovascular disease, they may be prescribed low-dose aspirin to prevent clotting.
For more symptomatic and complex cases of APS, a practitioner may prescribe the following:
- direct oral anticoagulants such as dabigatran (Pradaxa), rivaroxaban (Xarelto), apixaban (Eliquis) and edoxaban (Lixina and Savaysa);
- the anticoagulant Warfarin (Coumadin);
- fast-acting Heparin which is delivered by injection and often given to women wishing to get pregnant or have had a history of miscarriage;
- prednisone (used to suppress the immune system activity and inflammation); and
- for those with SLE who have APS, hydroxychloroquine (Plaquenil) can also add some protection against blood clots.

Complications of Antiphospholipid Syndrome
If left untreated, APS can cause serious conditions:
- Vascular Thrombosis, which may appear for the first time as a blood clot in an artery or vein, such as a deep vein thrombosis (DVT).
- Embolism, which is the blockage of a blood vessel that can be caused by a clot that has traveled in the blood stream from another location in the body. A pulmonary embolism occurs when a clot forms in a vein, then detaches and travels to the lungs .
- Heart valve disease due to “vegetation” growths or clots that prevent the valves of the heart from opening and closing properly.
- Renal disease due to clots in the kidney arteries, veins or glomeruli (similar to that found in lupus nephritis).
- Anemia, due to low iron uptake and autoimmune hemolytic anemia, in the form of a low red blood cell counts.
- Thrombocytopenia or (immune thrombocytopenia), which means a low platelet counts.
- Livedo reticularis, a lace-like or marbled rash that appears red or blue in color and appears right below the skin – usually seen in the legs and arms.
- Stroke or other neurological disorders such as embolic stroke (caused by a blood clot that travels to the brain) or cerebrovascular thrombosis (a blood clot that forms in the brain) can occur.
- Seizures, migraines and cognitive problems.
- Catastrophic APS may occur if multiple blood clots form throughout the body, damaging organs or causing organ failure. If an individual experiences catastrophic APS, they will be treated with high dosages of anticoagulants.
Women and APS
Women with APS are at particular risk of developing pregnancy complications. These complications are some of the “hallmarks” of APS and include:
- miscarriage;
- premature birth;
- pre-eclampsia;
- eclampsia;
- hemolysis, elevated liver enzymes, low platelet count or HELLP syndrome; and
- placental abruption.
Some women may be asked to avoid pregnancy. Individuals with pulmonary hypertension, for example, are at a particular high risk. “Preconception counseling” between a woman and her practitioner will help both understand the risks of becoming pregnant and what steps need to be taken to ensure a safe and healthy pregnancy and delivery.
Women who are pregnant will be closely monitored. Researchers recommend check-ups every two-to-four weeks before mid-gestation and every one-to-two weeks for the remainder of the pregnancy. If properly treated and managed, 70% of pregnant women with APS will deliver healthy babies.
Women who are currently taking estrogen for birth control or menopausal symptoms may be asked to stop taking these medications as they have been known to increase the risk for blood clots.

Managing Antiphospholipid Syndrome
If an individual is diagnosed with APS and is taking anticoagulants, blood may not clot as easily. It is best to take the following precautions to avoid excessive bleeding:
- shave with an electric razor rather than a blade;
- use a softer toothbrush and waxed floss to protect the gums;
- be extra cautious around sharp objects like scissors and knives; and
- avoid any activities or sports that may cause bruising or injury or may cause falling.
It is important to note that surgery can increase the risk for blood clots in individuals with APS. A healthcare practitioner should fully discuss the risks of surgery as needed.
An individual can also manage their APS by doing the following:
- quitting smoking or using tobacco products;
- keeping cholesterol and triglyceride levels low;
- managing a healthy weight;
- eating a healthy diet; and
- keeping blood pressure regulated and under control.
It is very important to speak with a healthcare practitioner about any other prescribed medications or supplements that may cause the anticoagulants to be less effective or interact in a dangerous way. It is also important ask about any dietary restrictions that can either increase or reduce the medication’s blood-thinning effect.
Individuals with APS who travel by air are also encouraged to get up and move around during flights. Individuals with APS who have to sit anywhere for long periods of time should stand and move as often as possible as well.
Conclusion
While there is no cure for antiphospholipid syndrome, there are very successful ways to manage and treat this condition. There are also several APS clinical trials being conducted globally – check ClinicalTrials.gov to find out more. Individuals diagnosed with APS should be mindful of new symptoms by keeping good medical records with dates and descriptions of symptom activity. Medications and outcomes should also be monitored and communicated to a healthcare practitioner as well as information about general wellness. As always, open and direct communication between the individual and their healthcare practitioner is critical to managing this condition.
References
Ahmadzadeh, N., Ahmadzadeh, Y., & Erkan, D. (2019). Top 10 series: Antiphospholipid syndrome and potential new treatments. Hospital for Specialty Surgery. Retrieved July 3, 2020 from https://www.hss.edu/conditions_top-ten-series-antiphospholipid-syndrome-potential-new-treatments.asp
Antiphospholipid syndrome. (n.d.). Mayo Clinic. Retrieved July 3, 2020 from https://www.mayoclinic.org/diseases-conditions/antiphospholipid-syndrome/symptoms-causes/syc-20355831
Antiphospholipid syndrome. (2020). Johns Hopkins Lupus Center. Retrieved July 3, 2020 from https://www.hopkinslupus.org/lupus-tests/antiphospholipid-antibodies/
Antiphospholipid syndrome. (2020). MedlinePlus. Retrieved July 3, 2020 from https://medlineplus.gov/ency/article/000547.htm
Antiphospholipid syndrome and acute HIV infection. (2010). Centers for Disease Control and Prevention. Retrieved July 3, 2020 from https://wwwnc.cdc.gov/eid/article/16/2/09-0728_article
Gardnier, C., Hills, J., Machin, S., & Cohen, H. (2013). Diagnosis of antiphospholipid syndrome in routine clinical practice. Lupus, 18-25. doi: 10.1177/0961203312460722. Retrieved July 3, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4108293/pdf/10.1177-0961203312460722.pdf
Martin, L. (2018, November 16). What is antiphospholipid syndrome? WebMD. Retrieved July 3, 2020 from https://www.webmd.com/dvt/what-is-antiphospholipid-syndrome
Park, S., Jang, S., Park, C., & Chi, H. (2016). Clinical application of revised laboratory classification criteria for antiphospholipid antibody syndrome: Is the follow-up interval of 12 weeks instead of 6 weeks significantly useful? BioMed Research International. Doi: 10.1155/2016/2641536. Retrieved July 3, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5005572/pdf/BMRI2016-2641526.pdf
Pons-Estel, G., Tincani, A., & Andreoli, L. (2016). The antiphospholipid syndrome in patients with systemic lupus erythematosus. Journal of Autoimmunity, 1-11. doi: 10.1016/j.aut.2016.10.004. Retrieved July 3, 2020 from https://www.researchgate.net/profile/Guillermo_Pons-Estel/publication/309360958_The_antiphospholipid_syndrome_in_patients_with_systemic_lupus_erythematosus/links/5cb9be12a6fdcc1d499fee73/The-antiphospholipid-syndrome-in-patients-with-systemic-lupus-erythematosus.pdf
Prima, F., Valenti, O., Hyseni, E., Giorgia, E., Faraci, M., Renda, E., De Domenico, R., & Monte, S. (2011). Antiphospholipid syndrome during pregnancy: The state of the art. Journal of Prenatal Medicine, 5(2), 41-53. Retrieved July 3, 2020 from
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3279165/pdf/prenatal-05-0041.pdf
Reddel, S. & Krilis, S. (1999). Testing for and clinical significance of anticardiolipin antibodies. Clinical and Vaccine Immunology, 6(6), 775-782. doi: 10.1128/CDLI.6.6.775-782. Retrieved July 3, 2020 from https://cvi.asm.org/content/6/6/775
Shiel, W. (n.d.). Antiphospholipid syndrome. MedicineNet. Retrieved July 3, 2020 from https://www.medicinenet.com/antiphospholipid_syndrome/article.htm#what_causes_antiphospholipid_syndrome
What is antiphospholipid syndrome? (2010). National Human Genome Research Institute. Retrieved July 3, 2020 from https://www.genome.gov/Genetic-Disorders/Antiphospholipid-Syndrome
Author: The KFL Team
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

