Allergies and Lupus
Both allergies and lupus are conditions driven by an overly reactive immune system, and both are seemingly on the increase. Are they related and why?
- Introduction
- What are the most common types of allergies?
- What are the symptoms of an allergic reaction?
- What causes allergies?
- Testing for Allergies
- Treating and Preventing Allergic Reactions
- Allergies Impact on Quality of Life
- In Conclusion

Introduction
An allergy occurs when an individual experiences a bad, defensive reaction to something that to most people would be considered harmless. In other words, allergies are an overly sensitive immune response to a substance that comes into contact with the body. The substance that triggers this response is called an allergen. Immune responses are incredibly complex because the body needs to, at the same time, defend itself without injuring itself too much. Yet, as anyone with lupus can attest, the body is not always successful in this!
Once the immune system has identified the potentially damaging antigen, it creates antibodies for it. These antibodies attach to mast cells, which are found in connective tissue. When the allergen comes in contact with the antibodies, the mast cells release histamines, which cause inflammation. This reaction can be anything from a sneeze or an itch to something more sinister such as severe diarrhea or even anaphylaxis. An individual who is triggered by allergens is said to be atopic because they have a tendency to develop hypersensitivity or atopic disease. Eczema (atopic dermatitis) is a common example.
If an individual has systemic lupus erythematosus (SLE) or another autoimmune disease, there is a tendency to have allergies as well. Atopic disease is also considered an immune disorder. Yu-Ping Hsiao et al., for example, found that individuals with lupus are up to two times more prone to experiencing atopic dermatitis and asthma than individuals who do not have lupus. Conversely, this same research found that individuals with atopic disease have a two-times greater risk for developing SLE … especially women. A study by C.G Parks and others found that individuals who developed childhood-onset allergies may also be at higher risk of developing lupus as opposed to individuals who did not develop allergies until adulthood.
.
What are the most common types of allergies?
The Asthma and Allergy Foundation of America (AAFA) lists the following most common types of allergies:
- Drug allergy: Prescription and over-the-counter medications can cause allergic reactions in individuals who are atopic. Common drug allergens include antibiotics, non-steroidal anti-inflammatories, chemotherapy drugs, and monoclonal antibodies.
- Food allergy: Common food allergens include dairy, eggs, fish – including shellfish, peanuts (which are technically not nuts – they are legumes), tree nuts, wheat and soy.
- Insect allergy: Insects with stingers including bees, wasps and hornets can cause allergic reactions. Fire ants are also a known allergen.
- Latex allergy: Triggers include balloons, surgical gloves, and even some bandages (plasters, band-aids).
- Mold allergy: Mold is a fungus with spores that travel by air. Alternaria, Aspergillus, Cladosporium and Penicillium are the most common fungi that can produce an allergic reaction.
- Pollen allergy: If an individual suffers from hay fever, they are allergic to the pollen on trees, other plants or even some fruits and vegetables. Fruits and vegetables such as apples, kiwi and celery contain proteins that are similar to those found in pollen and can potentially be allergenic.
- Pet allergy: It is actually the proteins found in animal dander, skin, saliva and even urine that can cause an allergic response. A pet dog or cat can also carry pollen or other allergens into a home after a romp or roll outside – the individual who reacts may not technically be allergic to their pet, but instead to “what the cat dragged in.”
It is important to note that celiac disease is technically not an allergy – it is an immune reaction to eating the protein gluten, which is found in wheat, barley and rye and affects the small intestine. When an individual with celiac comes in contact with gluten, the body creates antibodies, and these antibodies attack the entire body similar to any autoimmune disease and not just the gluten protein. National Institute of Diabetes and Digestive and Kidney Diseases estimates that approximately 1 in 141 people living in the U.S. have celiac disease – and most do not know it.
It cannot be ignored that there has been an increase in the prevalence of food allergies over the last several years, and children are particularly at risk. The organization Food Allergy Research and Education estimates that approximately 32 million Americans including almost 6 million children have food allergies. According to the Centers for Disease Control, food allergies in children alone increased by 50% between 1997 and 2011. Researchers Wenyin Loh and Mimi L. K. Tang found that in Western countries, the most common children’s food allergies include eggs, sesame, wheat, soy, tree nuts, fish, shellfish and cow’s milk with peanuts topping the list. In a large 2017 study of over 40,000 children published in the journal Pediatrics, Ruchi S. Gupta et al. determined that non-Hispanic African-American children have the risk of having multiple food allergies as opposed to non-Hispanic white children though the reason is not understood. Rudolf Valenta et all noted in their 2015 Gastroenterology article that these increased occurrences of food allergies may be due to the hygiene hypothesis which will be discussed later in this article.
Individuals with lupus who have allergies often report experiencing atopic dermatitis, conjunctivitis, allergic rhinitis and asthma as some of the most common manifestations. Gupta et al. reported that 55% of the individuals they studied also reported active SLE while experiencing allergy symptoms. According to Francisco Aceves-Avila and Verónica Benites-Godínez, individuals with SLE may also experience drug allergies – especially to sulfa. Individuals with lupus also experience more drug allergies than individuals with rheumatoid arthritis, another autoimmune disease.
.
What are the symptoms of an allergic reaction?
While the severity and duration can be different from individual to individual, the Mayo Clinic has identified the following most common symptoms of allergic reactions based on the allergen:
- Allergic Rhinitis (Hay fever): An allergy to plants and pollen can cause sneezing, eye irritation, nasal congestion and an itchy nose or roof of mouth.
- Food Allergy: Individuals with food allergies may experience swelling (face, tongue, lips, throat), hives, a tingly mouth and even anaphylaxis. Reactions to foods such as wheat, gluten and soy can cause these symptoms along with digestive upset (nausea, vomiting, diarrhea), red and flushed skin, abdominal pain, cramps, headache, nasal congestion and swelling of the face and throat.
- Insect Sting Allergy: Insect stings (bees, wasps) can cause hives, redness and swelling around the sting, compromised breathing (wheezing, coughing, tightness of the chest) and anaphylaxis.
- Drug Allergy: I, personally, am allergic to penicillin and sulfa. When I have taken either in the past, I have had hives, itching and face swelling. Rash, wheezing and anaphylaxis can also be symptoms of a drug allergy.
- Atopic Dermatitis (Eczema): This skin allergy can cause itching, red, flaking and peeling skin.
It is important to briefly discuss anaphylaxis since it can be a potentially life-threatening allergic reaction to so many allergens as noted above. Anaphylaxis occurs when an individual comes in contact with an allergen and the body goes into shock as a flood of chemicals is released. This flood of chemicals causes blood pressure to drop and airways to become restricted, resulting in difficulties with breathing. According to the Mayo Clinic, symptoms include hives and itching, and weak and rapid pulse, nausea and vomiting, a swollen tongue or throat and potentially fainting. Individuals who know they can go into anaphylaxis usually carry an epinephrine autoinjector with them, but even after she or he uses this, the individual without question needs to be seen at an emergency room immediately.
.
What causes allergies?
Hygiene Hypothesis
While are several theories about what may cause allergies – the most prolific is the “hygiene hypothesis” which also serves as the premise for subsequent theories. The hygiene hypothesis was developed in the 1980s and basically states that people who live in industrialized societies, while at less risk of infection, have a greater risk of developing allergies, asthma and autoimmune disorders. The more hygienic and developed the society, the fewer the germs and therefore the fewer the chances of developing the antibodies needed for immunity. The infectious burden is much higher in undeveloped societies, but individuals also have more antibodies and therefore more resistance to allergic and autoimmune conditions. Researchers Okada et al. in their 2010 article for The Journal of Translational Immunology suggest that this could explain why, for example, African Americans living in post-industrialized U.S. are at greater risk of developing SLE than someone living in underdeveloped West Africa.
The Microbiome
Staci Bilbo et al. discuss the “staggering” presence of allergic and autoimmune disease in post-industrialized societies and cite that for example, “more than one person in 1000 acquires lupus … one in 40 suffers from food allergies … one in 18 report symptoms of asthma … and approximately half of the population in the [U.S.] reacts against common allergens based on a skin test.” A possible explanation could be that individuals living in these post-industrialized societies have a much less diverse microbiome of the gut bacteria. Modern technologies such as antibiotics, antiseptics, and substituting formula for mother’s milk have negatively impacted the microbiome. Being hyper-clean and germ-free has almost completely eradicated some components of our gut bacteria, and other organisms like helminths. Helminths are worm-like parasites that live in the gut and the “good ones” are responsible for keeping the microbiome in balance. A microbiome that is out of balance may make an individual vulnerable to disease and produce allergic reactions. The relationship between gut health and immunity is one of the most intensely researched areas to date, and the implications for lupus, as well as allergies, are truly great!
Genetics
In 2013, National Institute of Health (NIH) scientists discovered a genetic link between allergic and autoimmune diseases. Though the study was conducted in mice, its results show promise. The scientists discovered a gene in B cells named BACH2 that has proven to be a “critical regulator of the immune system’s reactivity” and that “minor variations” in BACH2 can impact the immune system. Individuals who have a variation in BACH2 often have conditions such as asthma, allergies, Crohn’s disease, celiac disease, multiple sclerosis and type 1 diabetes. Though more research needs to be done, the scientists agree that this discovery may be the “first step in developing novel therapies for these disorders.”
.
Testing for Allergies
An allergy specialist (allergist) typically tests for allergies. If an individual has lupus, the allergist should join the team of healthcare practitioners currently developing lupus treatment plans to ensure the individual’s lupus is adequately managed. If an individual has cutaneous lupus and is experiencing a flare, for example, they may have to wait until the flare subsides in order to have a skin test performed.
The following types of allergy testing may be administered in order to properly diagnose an atopic condition:
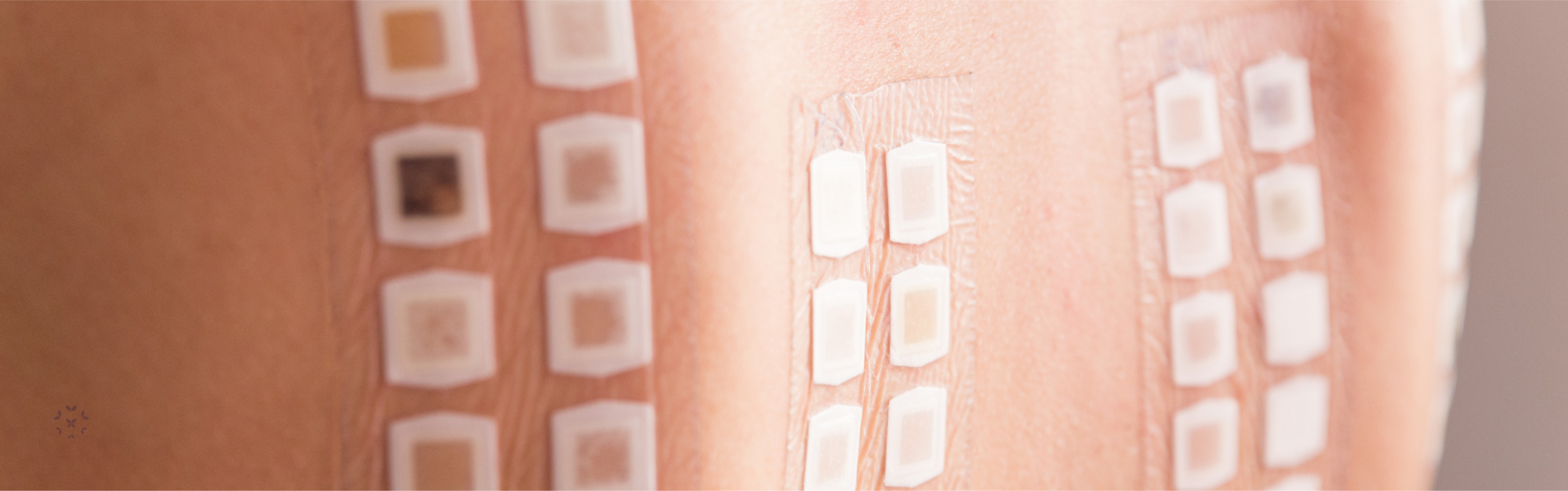
- IgE Skin Tests (often called a “prick” test): A small amount of an allergen is inserted into the surface of the skin via a small prick and is often done on the back and arms and is relatively painless. IgE is an antibody that is present if an individual is having a reaction to an allergen. If there is a reaction, the skin around the prick point will become swollen, itchy and red like a hive.
- Skin Scratch/Scrape Tests: If a prick test does not work, a small patch of the skin may be removed and the potential allergen rubbed on the area to check for a reaction.
- Patch Tests: A patch containing the suspected allergen is applied to an individual’s back for 24-72 hours to determine a reaction.
- Challenge Tests: Used most often to determine food allergies, an individual inhales or ingests a small portion of the food or even drug allergen under very close medical supervision.
- Blood Tests: Blood tests are sometimes used to determine an allergy when the individual either has a skin condition that will not allow for testing or when ingesting or inhaling an allergen may be unsafe. Blood tests look for the antibody IgE.
Linda Cox et al. reason that one of the pitfalls of allergy testing is that it can be subjective on the part of the healthcare practitioner administering and interpreting the tests – many practitioners are simply not familiar with the processes. Cox’s research also highlights the importance of taking an individual’s self-reported symptoms into consideration when a healthcare practitioner diagnoses an allergy. While testing may provide more definitive information, these tests can sometimes yield inaccurate results, often showing false positive results as opposed to false negative. The clinical history of an individual may provide the most important clues in determining what is truly an allergen.
According to the American College of Allergy, Asthma and Immunology, skin testing has been in use for over 100 years and is relatively safe. An allergist should work closely with an individual to make sure the testing done is appropriate and low-risk. If an individual needs challenge testing, an allergist should again work closely with that individual to determine the risks since this is a more invasive procedure. A healthcare practitioner should conduct testing in a manner that will not put the individual at risk.
.
Preventing and Treating Allergic Reactions
In the case of preventing food allergies in childhood, Valenta et all suggest a mother breast-feed her baby for up to the first six months if possible to prevent allergies. If breast-feeding is not possible, a high-risk child may be given hypoallergenic formula to stave off allergies. The best way to prevent allergic reactions to anything in general, however, is to avoid the known allergens as best as possible.
The AAFA also recommends taking medicines as prescribed and carrying an epinephrine auto-injector as well if needed in order to prevent or possibly treat a reaction. Wearing a medical alert bracelet will let others know of severe allergies in case you are unable to communicate. Keeping a diary of symptoms and triggers can also help healthcare practitioners determine what may be causing reactions and how to prevent them.
In the event an allergen cannot be avoided, the AAFA lists the following most common treatments for many common allergies. Make sure you discuss these with your healthcare practitioner as some may have an affect with your lupus medications:
- Over-the-Counter Allergy and Cold Medicines: Many of these medications contain aspirin or other NSAIDs, however, which can potentially pose an allergic risk.
- Nasal Corticosteroids: Nose sprays may reduce swelling, eye discomfort and congestion.
- Antihistamines: Antihistamines are often prescribed for seasonal allergies and can minimize sneezing, hives and itching.
- Mast Cell Stabilizers: These are eye drops and nose sprays that may keep an individual’s body from releasing histamine.
- Decongestants: Decongestants can reduce swelling and stuffiness in the nose and ears, but prolonged use can actually have the reverse
- Corticosteroid Creams and Ointments: Topical treatments can reduce itchiness and skin rash.
- Oral Corticosteroids. This treatment can reduce swelling, but do come with risks.
- Epinephrine: In an injectable device, epinephrine is given during life-threatening anaphylaxis.
- Allergy Shots: These shots contain bits of allergen and are often given to treat pollen, pet, dust and insect allergies in order to build tolerance.
- Sublingual Immunotherapy (SLIT): Used to treat dust mite, grass and ragweed allergies, SLIT contains a tiny bit of the allergen administered under the tongue in the hopes of building tolerance.
Food allergies are harder to treat. According to the AAFA, researchers are currently studying potential treatment options. The U.S. Food and Drug Administration (FDA) has recently approved the use of Palforzia, however, to help treat accidental exposure to peanuts and even anaphylaxis. Palforzia may be started in children between the ages of 4 and 12 and may be continued in children over the age of 4. This is not a cure, however. Peanuts must still be avoided. Oral immunotherapy and SLIT are currently under investigation, but their efficacy has yet to be conclusively proven. An allergist will work closely with an individual experiencing food allergies to determine the best course of care. Often avoidance is the only way.
If an individual has lupus, great care should be taken to make sure there are no contraindications with prescribed treatments. It is vital that an individual’s healthcare practitioners work as a team to make sure she or he is not at risk for developing complications. Advocating for one’s self – making sure to openly and confidently discuss any symptoms, current health condition and concerns – can also go far to ensure one receives the best care possible.

.
Allergies Impact on Quality of Life
Allergies should not be underestimated as they can greatly impact an individual’s life. Children can be particularly hard-hit when it comes to allergies, especially food allergies. Much like living with a chronic condition such as lupus, special care needs to be taken day-to-day in order to mitigate the potential risks of becoming severely ill. An allergy can also take a while to diagnose, much like a lupus diagnosis can. This can be a huge psychological burden to bear and huge source for anxiety.
Darío Antolín-Amérigo et al. studied how allergies impacted quality of life. They acknowledge the psychosocial implications of having allergies, in particular food allergies. Some parents reported not feeling confident in managing their child’s allergies, and children reported feeling anxious about food in general due to their limitations and the potential risk of reaction. Based on their review of the literature, this research emphasized the need for education, for not only the individual with the food allergy, but their caregivers as well – it is important for all involved to develop the right coping skills. Healthcare practitioners should work with the atopic individual as well as any caregivers, intervening when necessary and routinely evaluating the emotional well-being of all impacted. Cognitive behavioral therapy and working with a mental healthcare practitioner may be important for a holistic approach to a person’s allergies – especially if she or he also has lupus. Relying on support systems can also bring some peace of mind.
.
In Conclusion
We live in a world where allergies and autoimmunity are becoming more common. It is important to remember that healthcare practitioners and researchers are working hard to investigate the reasons why. There are lessons to be learned about the relationship between hypersensitivity and autoimmunity. Each is an example of the immune response overreacting in an unhealthy way. The more we can educate ourselves and carefully observe what causes these conditions in our lives – and communicate them effectively to our healthcare practitioners – the better we can all work toward effective treatments and eventual cures.
References
Aceves-Avila, F., & Benites-Godínez, V. (2008). Drug allergies may be more frequent in systemic lupus erythematosus than in rheumatoid arthritis. Journal of Clinical Rheumatology. Retrieved January 31, 2020, from https://www.ncbi.nlm.nih.gov/pubmed/18679134
American Academy of Allergy Asthma & Immunology. (n.d.). Allergy testing. Retrieved January 31, 2020 from https://www.aaaai.org/conditions-and-treatments/library/allergy-library/allergy-testing
Antolín-Amérigo, D., Manso, L., Caminati, M., de la Hoz Callaber, B., Cerecedo, I., Muriel, A., Rodríguez-Rodríguez, M., Barbarroja-Escudero, J., Sánchez-González, M., Huertas-Barbudo, B., & Alvarez-Mon, M. (2016). Quality of life in patients with food allergy. Clinical and Molecular Allergy. Retrieved January 31, 2020 from https://link.springer.com/content/pdf/10.1186/s12948-016-0041-4.pdf
Asthma and Allergy Foundation of America. (n.d.). Preventing allergic reactions and controlling allergies. Retrieved January 31, 2020 from https://www.aafa.org/prevent-allergies/
Asthma and Allergy Foundation of America. (n.d.). Types of allergies. Retrieved January 31, 2020 from https://www.aafa.org/types-of-allergies/
Australian Society of Clinical Immunology and Allergy. (2019). What is allergy? Retrieved January 31, 2020 from https://www.allergy.org.au/patients/about-allergy/what-is-allergy
Bilbo, S., Wray, G., Perkins, S., & Parker, W. (2011). Reconstitution of the human biome as the most reasonable solution for epidemics of allergic and autoimmune disease. Medical Hypotheses 77(2011), 494-504. doi:10.1016/j.mehy.2011.06.019.
Cox, L., Williams, B., Sicherer, S., Oppenheimer, J., Sher, L., Hamilton, R., & Golden, D. (2008). Pearls and pitfalls of allergy diagnostic testing: Report from the American College of Allergy, Asthma and Immunology Specific IgE Test Task Force. Annals of Allergy, Asthma & Immunology, 101(2008), 580-592.
European Centre for Allergy Research Foundation. (n.d.). Coeliac disease. Retrieved January 31, 2020 from https://www.ecarf.org/en/information-portal/allergic-diseases/celiac-disease/
Food Allergy Research & Education. (2020). Food Allergy 101. Retrieved January 31, 2020 from https://www.foodallergy.org/living-food-allergies/food-allergy-essentials/food-allergy-101
Gupta, R., Warren, C., Smith, B., Blumenstock, J., Jiang, J., Davis, M., Davis, M., & Nadeau, K. (2018). The public health impact of parent-reported childhood food allergies in the United States. Pediatrics. Retrieved January 31, 2020 from https://pediatrics.aappublications.org/content/pediatrics/142/6/e20181235.full.pdf
Hsiao, Y., Tsai, J., Muo, C., Tsai, C., Sung, F., Liao, Y., Chang, Y., & Yang, J. (2014). Atopic disease and systemic lupus erythematosus: An epidemiological study of the risks and correlations. International Journal of Environmental Research and Public Health. Retrieved January 31, 2020 from https://www.mdpi.com/1660-4601/11/8/8112
Loh, W., & Tang, M. (2018). The epidemiology of food allergy in the global context. International Journal of Environmental Research and Public Health. Retrieved January 31, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6163515/pdf/ijerph-15-02043.pdf
Mayo Clinic. (n.d.). Allergies. Retrieved January 31, 2020 from https://www.mayoclinic.org/diseases-conditions/allergies/symptoms-causes/syc-20351497
Mayo Clinic. (n.d.). Anaphylaxis. Retrieved January 31, 2020, from https://www.mayoclinic.org/diseases-conditions/anaphylaxis/symptoms-causes/syc-20351468
National Institutes of Health. (2013). NIH scientists find link between allergic and autoimmune diseases in mouse study. Retrieved January 31, 2020 from https://www.nih.gov/news-events/news-releases/nih-scientists-find-link-between-allergic-autoimmune-diseases-mouse-study
Okada, H., Kuhn, C., Feillet, H., & Bach, J. (2010). The ‘hygiene hypothesis’ for autoimmune and allergic diseases: An update. The Journal of Translational Immunology. 160, 1-9. Retrieved January 31, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2841828/pdf/cei0160-0001.pdf
Parks, C., Biagini, R., Cooper, G., Gilkeson, G., & Dooley, M. (2010). Total serum IgE levels in systemic lupus erythematosus and associations with childhood onset allergies. Lupus, 19(14), 1614-16622. Retrieved January 31, 2020 from https://journals.sagepub.com/doi/abs/10.1177/0961203310379870
Roychoudhury, R., Hirahara, K., Mousavi, K., Clever, D., Klebanoff, C., Bonelli, M., Sciume, G., Zare, H., Vahedi, G., Dema, B., Yu, Z., Liu, H., Takahashi, H., Rao, M., Muranski, P., Crompton, J., Punkosdy, G., Bedognetti, D.,… Restifo, N. (2013). Bach2 represses effector programmes to stabilize Treg-mediated immune homeostasis. Nature, 498(7455), 506-510. Retrieved January 31, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3710737/
S. Food and Drug Administration. (2020, January 31). FDA approves first drug for treatment of peanut allergy in children. [Press release]. https://www.fda.gov/news-events/press-announcements/fda-approves-first-drug-treatment-peanut-allergy-children
Valenta, R., Hochwallner, H., Linhart, B., & Pahr, S. (2015). Food allergies: The basics. Gastroenterology, 148(6), 1120-1131. Retrieved January 31, 2020 from https://www.ncbi.nlm.nih.gov/pubmed/25680669.
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

